Americans spent a record $158 billion on their pets in 2025. We buy them grain-free kibble, orthopedic beds, and birthday outfits. We call them family. And yet, according to nearly two decades of veterinary research, more than half of our dogs and cats are carrying enough extra weight to shorten their lives.

Pet obesity is not a cosmetic problem. Veterinary science classifies it as a clinical disease — one linked to arthritis, diabetes, respiratory failure, and a measurable reduction in lifespan.
The Association for Pet Obesity Prevention (APOP) has been tracking this issue since 2005, and their data tells a clear story: the problem is widespread, it is getting worse, and most pet owners do not realize it affects their own animal.
This article pulls together more than 30 statistics from APOP surveys, Banfield Pet Hospital records, Nationwide Insurance claims data, peer-reviewed veterinary studies, and the American Pet Products Association (APPA) to give you the most complete picture of pet obesity in the United States today.
Key Takeaways
- Roughly 59% of dogs and 61% of cats in the U.S. are classified as either overweight or obese based on veterinary body condition assessments.
- The percentage of overweight dogs visiting Banfield Pet Hospitals more than doubled between 2011 and 2020, rising from 16% to 34%. Cats followed a similar trajectory, climbing from 18% to 38%.
- Obesity can shorten a dog’s life by up to 2.5 years, according to a landmark study of age-matched Labrador Retrievers.
- Nationwide Insurance pays out more than $69 million per year in obesity-related veterinary claims — from a pool of just 700,000 insured pets, which represents fewer than 2% of all cats and dogs in the country.
- In APOP’s most recent survey, released in March 2026, only one in four dog owners and fewer than one in five cat owners who tried to help their pet lose weight reported lasting success.
- An overwhelming 95% of veterinary professionals recognize obesity as a disease, but 87% admit that concern about a client’s reaction has influenced whether or how they raise the subject.
How Pet Obesity Is Measured
Before diving into the numbers, it helps to understand how veterinarians define and measure obesity. They use a system called the Body Condition Score (BCS), typically measured on a 9-point scale.
A score of 4 or 5 is considered ideal. A score of 6 or 7 means the animal is overweight — roughly 10% to 20% above ideal body weight. A score of 8 or 9 means the animal is clinically obese, at 30% or more above ideal.
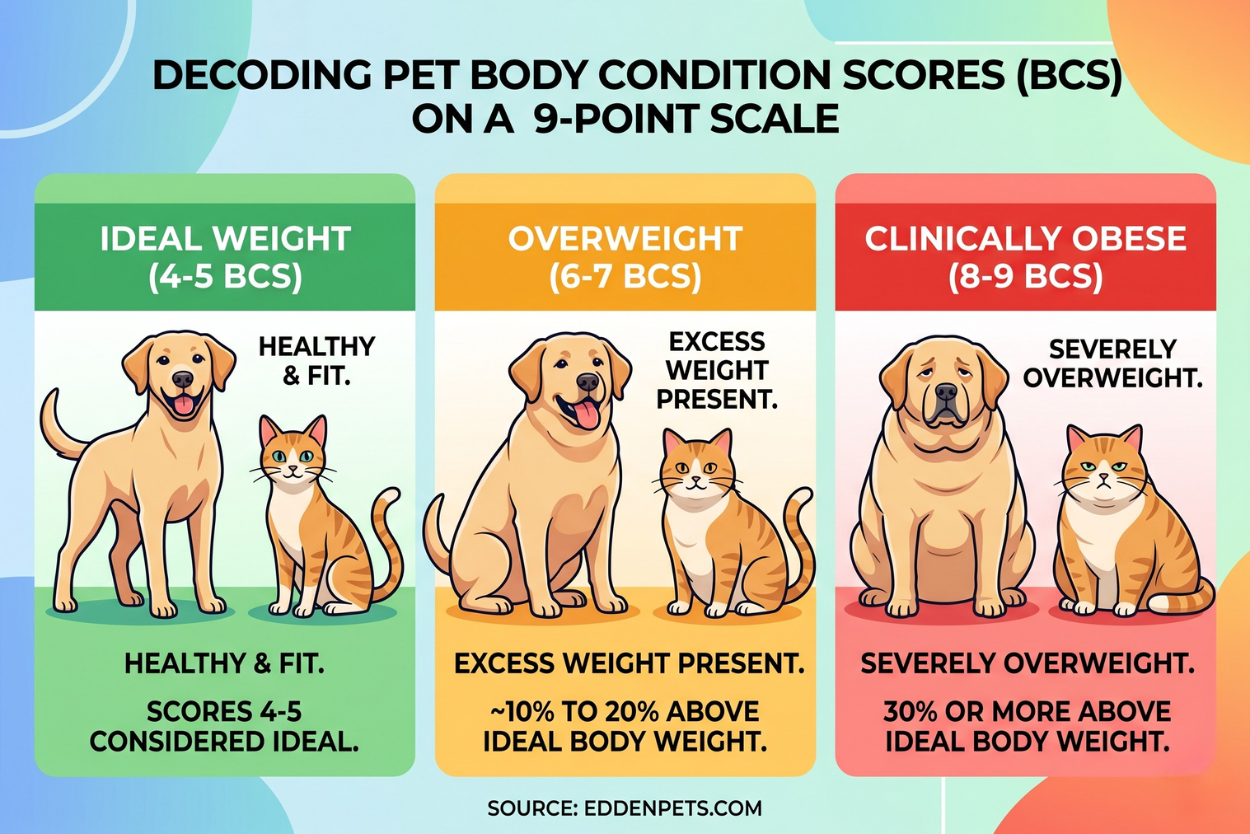
The assessment involves both visual examination and hands-on evaluation. A veterinarian checks the animal’s silhouette from above and from the side, looking for a visible waist and abdominal tuck.
They also feel for the ribs. In a healthy-weight animal, the ribs are easy to feel through a thin layer of tissue. In an overweight animal, they are buried under noticeable padding. In an obese animal, they may be nearly impossible to locate.
BCS is not perfect — dogs span a nearly 40-fold range in body mass from smallest to largest breeds, and thick coats can make visual evaluation less precise — but it remains the most practical and widely used clinical tool available.
Prevalence: How Bad Is the Problem?
1. Approximately 59% of U.S. dogs are overweight or obese.
Based on APOP’s most recent clinical prevalence survey, nearly six out of every ten dogs in the country are carrying more weight than is healthy for them. Among those, about 37% fall into the overweight category (BCS 6–7) and roughly 22% are classified as obese (BCS 8–9).
2. Approximately 61% of U.S. cats are overweight or obese.
Cats are even worse off than dogs. About 28% are classified as overweight and a full 33% are obese. Cats are not just heavier on average — they are more likely to be at the severe end of the scale.
3. An estimated 50 million dogs and 45 million cats in the U.S. are above a healthy weight.
The APPA reported that around 71 million U.S. households owned at least one dog in 2025, and roughly 53 million households had at least one cat. The total U.S. dog population is estimated at 87 to 90 million, with cats numbering 74 to 76 million. Apply the APOP prevalence rates, and the sheer scale of the problem comes into focus.
4. Obesity peaks during the “mature” life stage in both dogs and cats.
A large-scale study published in Preventive Veterinary Medicine in late 2024 examined the medical records of nearly 4.9 million dogs and 1.3 million cats seen at Banfield Pet Hospital locations between 2020 and 2023. Among mature dogs, 50.1% were overweight and an additional 12.6% were obese. Among mature cats, 44.8% were overweight and 21.7% were obese.
5. Weight problems that start early tend to persist for life.
That same Banfield study found that weight problems that start early tend to persist for life. Dogs who are overweight during their growth phase are 1.85 times more likely to be overweight as adults. For cats, the odds ratio was 1.52. This underscores the importance of establishing healthy weight habits from puppyhood and kittenhood onward.
6. Minnesota has the highest documented dog obesity rate of any U.S. state, at 41%.
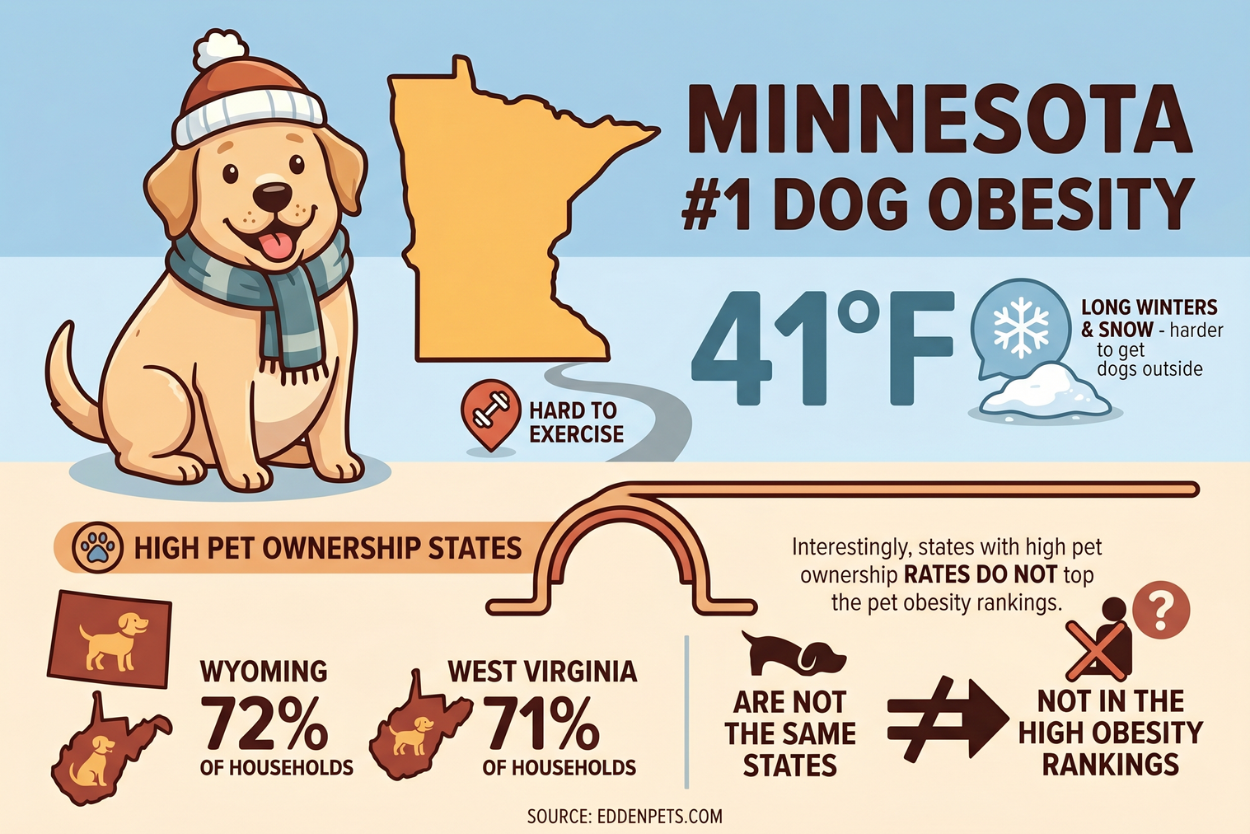
The long winters and months of snow and ice likely play a role — it is simply harder to get dogs outside for adequate exercise during a significant portion of the year. Interestingly, the states with the highest pet ownership rates — like Wyoming (72% of households) and West Virginia (71%) — are not the same states that top the pet obesity rankings.
Trends: How Did We Get Here?
7. The percentage of overweight dogs at Banfield Pet Hospitals more than doubled in a decade, rising from 16% in 2011 to 34% in 2020.
This long-term trend data from one of the largest veterinary chains in the country makes the trajectory unmistakable. The problem was growing steadily well before the pandemic arrived.
8. Overweight cats at Banfield clinics climbed from 18% to 38% over the same period.
Cats followed an even steeper trajectory than dogs. In both species, the rate more than doubled in less than a decade, driven by structural factors like larger portion sizes, a culture of treat-giving, and declining physical activity.
9. In APOP’s 2018 clinical survey, 55.8% of dogs and 59.5% of cats were classified as overweight or obese. By 2022, those figures had risen to 59% and 61%.
APOP’s annual surveys show that obesity rates among U.S. pets have hovered above 50% since at least 2010, and the trend has been gradually upward. The pandemic years accelerated the climb — with owners home full-time, pets had near-constant access to treats and structured exercise routines broke down — but the trajectory was already established.
10. Between 2022 and 2023, some pet obesity categories showed a slight decrease for the first time.
The 2024 Banfield study noted that the prevalence of overweight conditions in dogs and obese conditions in both species dipped slightly in certain life stages. It is far too early to call this a turning point, but it may be the first sign that awareness campaigns are starting to work.
11. 82% of U.S. dogs receive treats at least once every day.
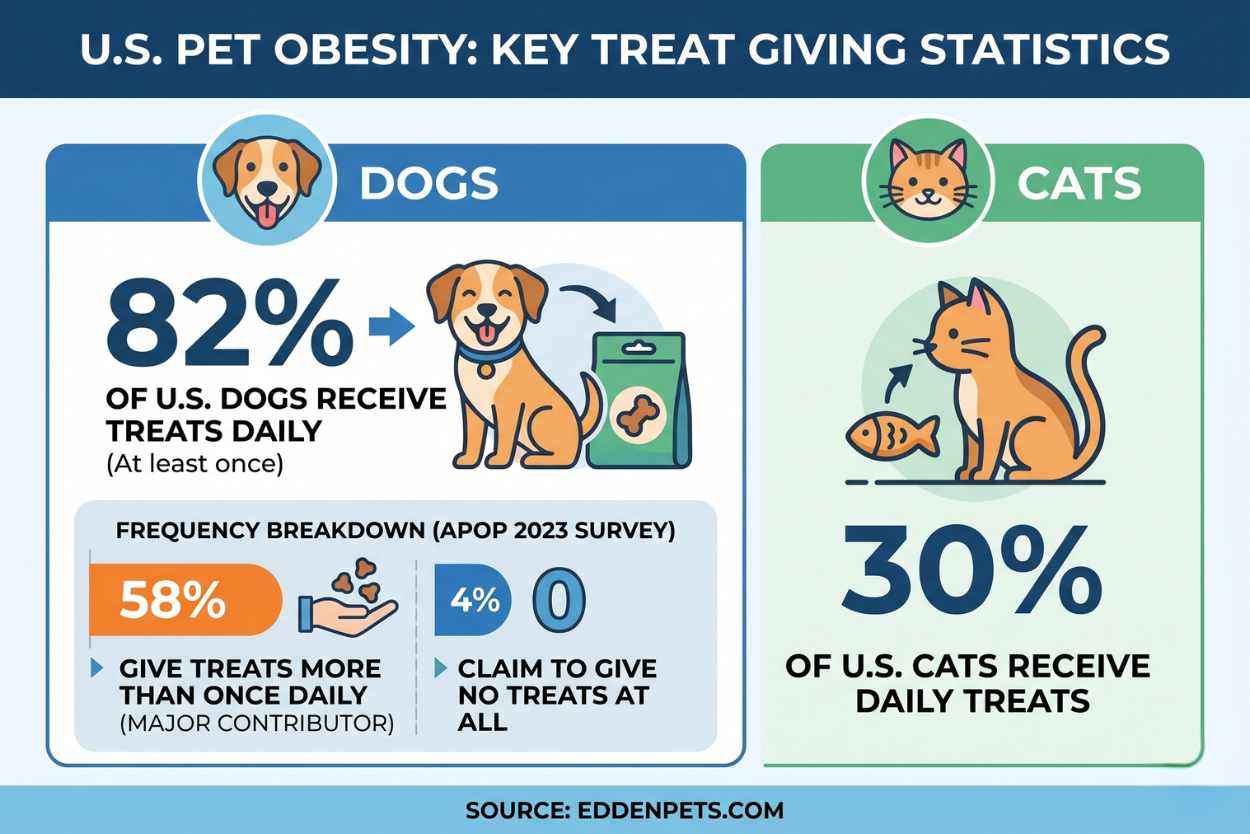
Treat-giving habits are a major contributor to the problem. In APOP’s 2023 survey, 58% of dog owners reported giving treats more than once daily. For cats, 30% received daily treats. Only 4% of dog owners claimed to give no treats at all.
12. 17% of dog owners admit to sharing their own food with their pets “usually” or “always.”
While about 25% of dog owners said they never shared human food, a significant minority acknowledged doing it routinely. Table scraps and shared snacks add untracked calories that compound over time.
The Perception Gap: Why Owners Don’t See It
13. In 2023, only 17% of dog owners acknowledged that their pet was overweight.
This is one of the most striking findings in APOP’s 2023 survey. Clinical data shows the real rate is closer to 59%, which means the vast majority of owners with overweight dogs do not realize it.
14. Only 28% of cat owners acknowledged their pet was overweight in 2023.
With clinical prevalence at 61%, the gap between perception and reality is enormous for cat owners as well. APOP researchers have coined the term “the fat gap” — when overweight becomes the norm in a population, people lose the ability to recognize what a healthy weight looks like.
15. Among owners whose pets were clinically overweight or obese, 32% classified them as “normal.”
Even more concerning, 9% of owners with obese pets — animals scoring 8 or 9 on the body condition scale — still believed their pet was in normal condition. They simply did not see it.
16. By 2024, owner awareness improved: 35% of dog owners and 33% of cat owners recognized their pet was overweight.
In APOP’s 2024 survey, recognition roughly doubled for dog owners compared to the previous year. Whether this reflects genuine improvement or survey variation remains to be seen, but the direction is encouraging.
17. Only 45% of dog owners and 40% of cat owners are familiar with body condition scoring.

Despite BCS being the standard tool for assessing pet weight, fewer than half of owners have even heard of it. This limits their ability to evaluate their own pet’s condition at home.
18. Just 27% of dog owners and 19% of cat owners recall their veterinarian ever providing a specific body condition score.
Over half of both groups said they had never received a BCS assessment from their vet. This represents a significant missed opportunity for early intervention.
19. 84% of veterinary professionals report that at least one client has appeared embarrassed or angry when told their pet is overweight.
This creates a chilling effect. Many veterinarians begin to soften their language, avoid the topic entirely, or wait for the owner to bring it up first — even though the problem is clinically significant.
20. Only 12% of pet owners say they have ever felt uncomfortable when a vet mentioned their pet’s weight.
The disconnect is striking. Veterinarians are significantly overestimating the backlash. In fact, 76% of owners said they believed their vet would be comfortable having the weight conversation. Both sides want to talk about it. Neither side thinks the other one does.
21. 95% of veterinary professionals recognize obesity as a disease, but 87% admit that concern about client reactions has influenced how they raise the topic.
APOP’s 2025 survey, released in March 2026, confirmed this communication breakdown. The clinical knowledge exists. The willingness exists on both sides. But a single awkward interaction can quiet a dozen necessary conversations.
Breeds and Risk Factors
22. 62.7% of Golden Retrievers and 58.9% of Labrador Retrievers are classified as overweight or obese.
One APOP survey found these two of America’s most popular breeds to be among the most affected. Other high-risk breeds include Pugs (statistically the most obese breed overall), Cocker Spaniels, Dachshunds, Beagles, Rottweilers, and Shetland Sheepdogs.
23. German Shepherds had the lowest obesity rate among common purebreds, at just 2.1%.
The contrast with Labs and Goldens is dramatic and points to the significant role genetics play in obesity risk across different breeds.
24. A gene mutation in Labrador Retrievers is directly linked to increased food motivation and 7–8% more body fat per copy.
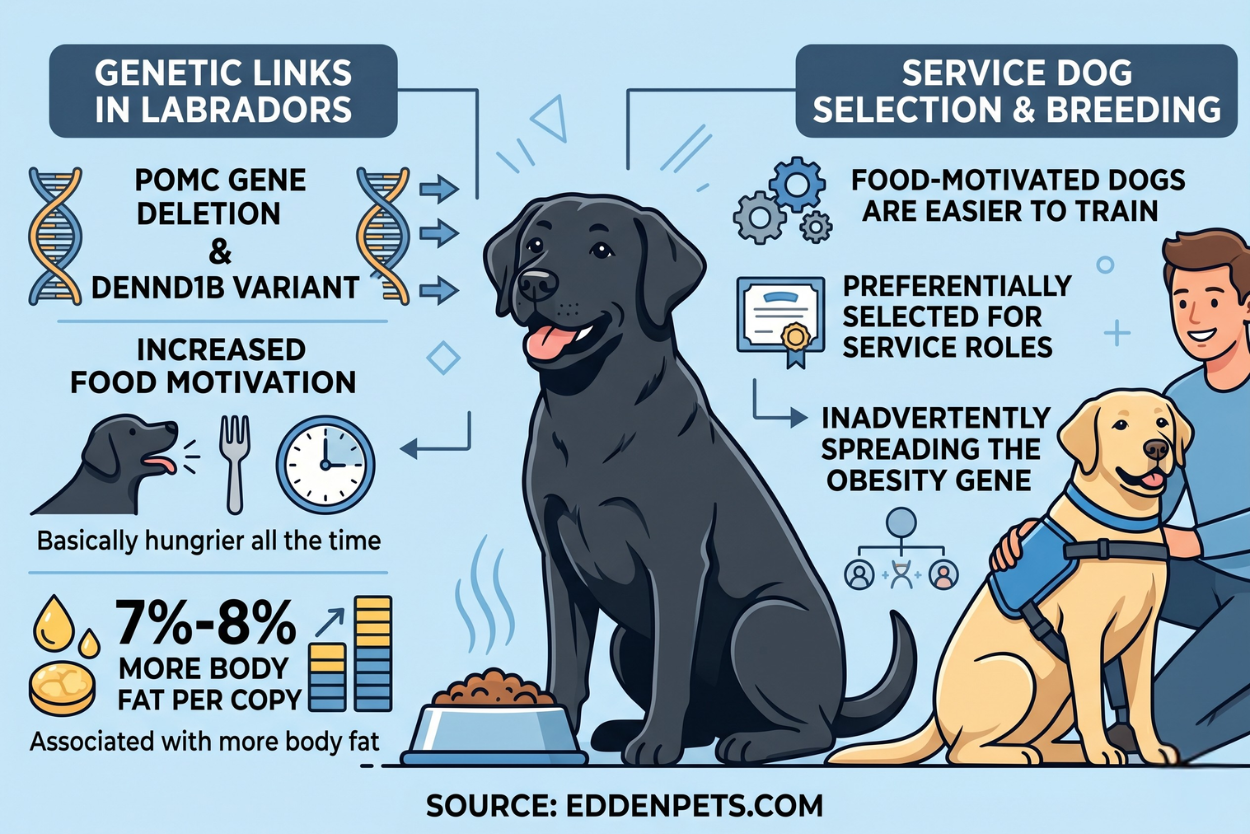
Researchers at the University of Cambridge, working with data supported by the Morris Animal Foundation, identified a deletion in the POMC gene that makes affected Labs essentially hungrier than other dogs, all the time.
The same team found that a variant of the DENND1B gene was associated with 7% to 8% more body fat per copy. Because food-motivated dogs are easier to train, they were preferentially selected as service dogs — inadvertently perpetuating the obesity gene through breeding programs.
25. Neutered male dogs are approximately 2.6 times more likely to become overweight or obese than intact males.
Spayed females face about 1.5 times the risk compared to intact females. These findings have been consistent across multiple studies. This is not an argument against spaying or neutering — the health benefits are well established — but it is a strong argument for adjusting diet immediately after the procedure.
26. Male cats post-neutering need 20–30% fewer calories, but experience increased appetite.
Hormonal changes create a perfect setup for rapid weight gain unless owners proactively reduce portion sizes. This makes the post-neutering period one of the most critical windows for obesity prevention in cats.
Health Consequences
27. Obesity can shorten a dog’s life by up to 2.5 years.
A landmark study of age-matched Labrador Retrievers found that dogs maintained at a lean body condition lived a median of 2.5 years longer than their overweight counterparts from the same litters.
For a breed with a typical lifespan of 10 to 14 years, that is a substantial loss. Other research has estimated that even moderate excess weight can reduce a dog’s lifespan by 6 to 12 months.
28. Obese cats experience roughly a 50% decrease in insulin sensitivity.
This makes diabetes mellitus one of the most common obesity-related diagnoses in felines. Cat insulin can cost up to $150 per month, and that does not include the cost of syringes, veterinary monitoring, or prescription food.
29. Overweight cats are approximately 4 times more likely to develop urinary issues than cats at a healthy weight.
Bladder and urinary tract disease is the number one obesity-related insurance claim for cats, according to Nationwide Insurance data. For dogs, arthritis tops the list.
30. Excess weight increases anesthetic risk and makes surgery more difficult and dangerous.
Fat tissue absorbs anesthetic drugs, making dosing less predictable and recovery slower. Surgeons must work through layers of adipose tissue to reach the target organ, and even routine procedures like dental cleanings carry elevated risk in obese pets.
One of the more dangerous conditions specific to overweight cats is hepatic lipidosis — when an obese cat stops eating for any reason, the body mobilizes stored fat faster than the liver can process it, potentially causing organ failure.
The Financial Cost
31. Nationwide Insurance pays out more than $69 million per year in obesity-related veterinary claims.

And this figure comes from a pool of just 700,000 insured pets. The United States is home to approximately 180 million pet dogs and cats combined, and fewer than 4% carry insurance. If 700,000 insured animals generate $69 million in obesity claims, the implied national burden is potentially in the billions of dollars annually.
32. Obesity-related conditions now account for 20% of all Nationwide pet insurance claims, up 24% over eight consecutive years.
The share of claims tied to obesity has risen steadily year after year. For dogs, the leading obesity-related diagnosis is arthritis. For cats, it is bladder and urinary tract disease. Other frequent claims include ligament injuries, digestive problems, diabetes, respiratory conditions, and various cancers.
33. Hip dysplasia surgery in dogs costs between $3,500 and $7,000 per hip.
According to veterinary cost data, the individual treatment costs for obesity-related conditions add up quickly. Cruciate ligament repair averages around $3,480. Diagnosing diabetes in a cat can run $2,400 or more when you include blood work, urine tests, and the first several months of insulin.
Even relatively common problems like arthritis management ($966 average) and digestive issues ($850 average) become expensive when they are chronic conditions requiring ongoing treatment.
34. The financial argument for prevention is straightforward: weight management costs a fraction of treating the diseases obesity causes.
A therapeutic weight-loss diet might cost modestly more than standard food, but it is far cheaper than a single emergency surgery. Maintaining a healthy weight through proper feeding and regular exercise remains the most cost-effective health intervention a pet owner can make.
Weight Loss: What Works and What Doesn’t
35. Only 1 in 4 dog owners who tried to help their pet lose weight reported lasting success.
APOP’s 2025 survey, released in March 2026, delivered this sobering finding. For cat owners, the results were even worse — fewer than 1 in 5 reported their pet reaching and maintaining a healthy body condition.
36. 58% of all pet owners are actively trying to help their pet lose weight — yet most are failing.
The survey found that 63% of dog owners and 45% of cat owners were making an effort. The problem is not motivation. People are aware and they are trying. The effort is just not producing results.
37. Only 22% of dog owners and 35% of cat owners have used a therapeutic weight-loss diet.

Therapeutic diets are specifically formulated to support fat loss while preserving muscle mass and managing the metabolic slowdown that accompanies calorie restriction. They are among the most effective tools available, yet the vast majority of owners rely on simply feeding less of their regular food — an approach that often leads to nutrient imbalances and does not address the biological factors that drive weight regain.
38. APOP’s position: pet obesity is a disease, not a discipline issue.
When four out of five cat owners cannot achieve lasting weight loss for their pet despite genuine effort, the failure is systemic, not personal. The barriers are biological, psychological, and structural, and most weight-loss plans do not come close to addressing all three.
APOP has also noted growing owner interest in medical interventions for pet weight management, a trend the organization plans to track in future research.
What Pet Owners Can Do: An Evidence-Based Approach
The statistics above can feel overwhelming, but the core actions that make a difference are straightforward.
Start with a number, not a guess. Ask your veterinarian for a specific Body Condition Score at every visit. Do not settle for vague reassurances. Request the number on the 9-point scale and ask what your pet’s ideal weight range should be. If your vet does not bring it up, you bring it up. The data shows that most owners are receptive to this conversation, even if some veterinarians hesitate to initiate it.
Learn to assess body condition at home. APOP and the World Small Animal Veterinary Association (WSAVA) both publish free body condition charts for dogs and cats. These are simple visual guides that show you what each BCS score looks like from above and from the side. Check your pet’s condition every couple of months between vet visits.
Get a calorie target. The feeding guidelines on most pet food bags tend to overestimate how much an animal needs. Ask your veterinarian to calculate a specific daily calorie target based on your pet’s ideal weight, age, activity level, and reproductive status. This is especially important after spaying or neutering.
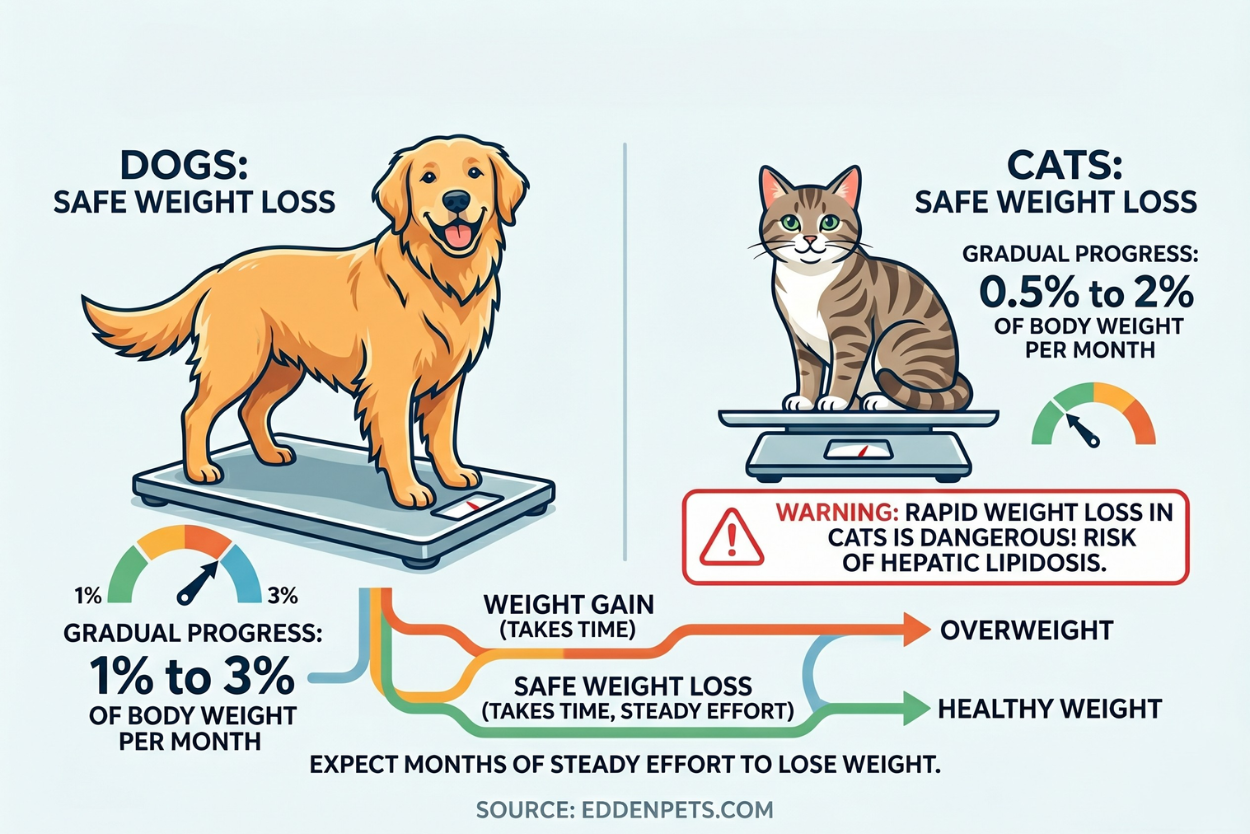
Be patient. Safe weight loss is slow. Dogs should lose 1% to 3% of their body weight per month. Cats should lose 0.5% to 2% per month. Rapid weight loss in cats is especially dangerous because of the risk of hepatic lipidosis. If it took months or years for your pet to gain the weight, expect months of steady effort to take it off.
Rethink treats. With 82% of dogs receiving treats at least once a day, this is one of the most controllable variables. You do not have to eliminate treats entirely, but consider switching to low-calorie options and counting treat calories as part of the daily total rather than treating them as extras.
If previous attempts have stalled, ask about therapeutic diets. Over-the-counter “light” or “weight management” foods are not the same as veterinary therapeutic weight-loss diets. The latter are specifically formulated to maintain satiety and preserve lean muscle during calorie restriction. They are one of the most effective tools available, yet fewer than one in four dog owners have tried one.
Weigh regularly. Step on the scale with your pet every two to four weeks during active weight loss, or use the scale at your veterinary clinic. Tracking progress keeps you accountable and helps your vet adjust the plan if things plateau.
Looking Ahead
Pet obesity in America is a problem measured in decades, not news cycles. APOP has been collecting data since 2005, and in nearly every year since, the numbers have moved in the wrong direction.
More than half of the nation’s dogs and cats are overweight. Most owners do not realize it. Most weight-loss attempts fail. And the veterinary profession, despite recognizing the severity of the issue, has struggled to communicate it consistently.
But there are real reasons for cautious optimism. Owner awareness, while still far too low, improved measurably between 2023 and 2024. Veterinary organizations are increasingly framing obesity as a clinical disease rather than a lifestyle choice, which opens the door to more systematic treatment approaches.
The paradox at the heart of this issue has not changed. We love our pets more than ever. We spend more on them than ever. And we are, with the best of intentions, feeding too many of them into early graves. The good news is that the single most important step is also one of the simplest: an honest conversation with a veterinarian, a number on a scale, and the willingness to hear it.